A few months ago, I was sat in a paediatric network meeting where we were listening to a fantastic DSN talking passionately about the transitional clinic and support her service offers to YPWD. The scope and range of the discussions were vast and the overwhelming sense of a desire to support all the children and young people living with diabetes that every person in the room held was palpable.
One discussion in particular left me pondering. The discussion was around safety. Keeping children and young people safe when supporting a wide range of management regimes. This in turn led me to think about how we manage migration between insulin management styles. (This wasn’t discussed or raised at the time – it is purely born from reflection upon the day’s discussions.)
There are some situations where using an insulin pump regime to manage diabaetes may, for a myriad of reasons, no longer be a safe for a person to manage their diabetes. Equally, a small cohort may not be safe using MDI. How do we support transitions between regimes without demotivating the person living with diabetes? How do we support them to not view a switch as a failure? Or a negative judgement?
Perception is a tricky business. Owing to the reletively small number of people managing their diabetes with technologies like insulin pumps and CGMs, it may be viewed as the “Champions’ League” of diabetes management. The holy grail to which all should aspire and hope to gain. Certainly with all the talk about using time in range as a new measure of diabetes management, the prevailing wind seems to be to push more toward tech useage, especially as time in range would be fairly onerous to prove without some form of either CGM or FlashGM. Someone using MDI to manage may not be interested in promotion to this league, but feel they are perhaps not ‘diabetesing enough’ if they decide to eschew the choice.
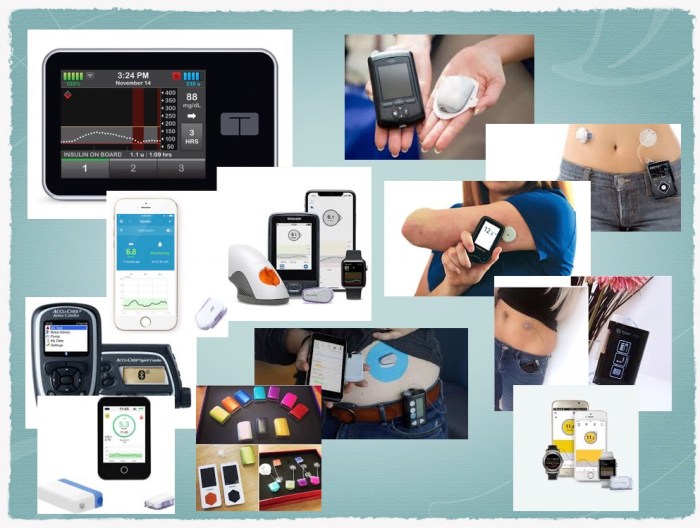 So much technology, but is it always best?
So much technology, but is it always best?
And so we have, without ever intending to, a heirachy of management styles. The impact of this is somewhat depressing. If we want to be able to support our children and young people to truly gain confidence and independence to live the lives they desire, surely it would be better to deliver messages that reinforce the truth that nothing is static. What works for you today, may not be suitable to meet your needs next week, month, or year. Just because you’ve used one particular regime for a number of years or decades, doesn’t preclude someone from trying something different.
Returning to the question of safety, I do not envy the HCPs who need to make these calls. It is, sadly, a reality of their workload, and I know these are the children and young people over whom they loose sleep. Imposed regime changes in these instances are not entered into lightly. Hours and hours of HCP support will have been dedicated to these cases. The priority of HCPs caring for someone who is struggling on every level is to keep them safe. It is this driver that leads to the suggestion of changing the status quo. I believe if the shifts between regimes were not seen as “failing” or “going backwards” or “levelling up”, then this supportive intervention would be viewed as a positive, rather than a negative.
The amount of times I have had discussions with people who just need a break from the endless data information they are streamed from devices (be it apps to monitor bgs, to alarms from cgms) but they feel unable to take that break for fear of loosing funding or having access to kit “downgraded”. Let’s be honest – to be “on it” all the time with diabetes mangement is an entirely unrealistic expectation. But the weight of responsibility to maintain to an unrealsitic expectation is collosal. I have lost count of the amount of times I’ve spoken to adults / teens / parents and they have, in hushed tones, “confessed” that they have “gone back” to using MDI to manage diabetes. My response to these confessionals is consistant – are you happy? Because when the answer to that question is yes, using MDI rather than CSII should never be viewed as a retrograde move. We need to be much better at delivering the message that one regime will not be a universal solution for all. That fluctuation between management styles is absolutely a personal choice and something that should always remain in one’s diabetes management armoury.
It is also important to acknowledge that in some circumstances it is affordability that denies access to specific regimes. And that properly sucks. Any of us who live with privilege has a responsibility to lobby the device companies to reduce costs and to open up access to as many as possible to be able to use tech safely and willingly. Whilst also remembering that everyone should have their own wishes respected and valued. Maybe then we will see more people comfortable and confident with the management regime they choose to use, not one they have been forced to. No one chooses to need to manage diabetes. Therefore, the very least that should be on offer is flexible options to best marry needs at a given time.

Pingback: No Hierarchy. No Judgement. Just Options.
The blog discusses the importance of having no hierarchy in diabetes management, emphasizing that everyone should feel free to choose their management style without fear of judgment. The author reflects on how transitioning between different management options, like insulin pumps and multiple daily injections (MDI), should be seen as a personal choice rather than a failure. This approach fosters confidence and supports individual needs in managing diabetes.
As a travel tip, using the <a href=”https://axacool.com” target=”_blank”> AXACOOL insulin cooling case</a> is crucial for those with diabetes. It ensures that insulin remains at the proper temperature during trips, allowing for more flexibility and peace of mind while navigating different management styles. https://axacool.com/
Summary of the Blog:
Comment:Great insights! It’s so important to foster an environment of acceptance and understanding in diabetes management. For those traveling or on the go, the Axacool insulin cooling case is a fantastic option to keep insulin at the right temperature, ensuring effective management wherever you are. Check out the full post here. http://www.axacoo.com